Tuberculosis in Modern Britain
What It Is, Why It’s Back, and What It Means
Introduction
TB has been around in Britain since the Iron Age. Did you know that? An early case was found in the bones of a person from that time, which are now on show at the Museum of East Dorset. It serves as a potent reminder that this illness has affected people for thousands of years (Bournemouth University, 2021). The bacterium Mycobacterium tuberculosis causes TB. Even though it can be severe, the good news is that it is both preventable and treatable. That gives us hope, especially since TB is still one of the world's deadliest infectious diseases (Tobin & Tristram, 2024).
As of 2025, TB remains a significant health issue in the UK. After many years of declining numbers, cases in England increased by 13% between 2023 and 2024 (UK Health Security Agency, 2025). This worrying increase has set back significant progress and requires urgent attention. An increasing number of health experts are now keeping a close eye on this since it appears quite like the rise in tuberculosis cases around the world after the COVID-19 pandemic. This article discusses what tuberculosis is, how it spreads, and why it remains a significant issue today. Most people who want to learn more about TB in the UK in 2025 will find clear and helpful information here. This includes students, healthcare professionals, and individuals interested in learning more.
Background / Context – Historical or Situational Overview
TB has been part of Britain's story for centuries. Long before we called it "tuberculosis," people knew it as "consumption"—a slow, wasting illness that claimed thousands of lives, especially in the 19th century. In Victorian times, TB was romanticised in poetry and novels, but in reality, it was feared for its deadly nature and its close association with poverty (Cooper, 2008).
By the early 1900s, TB had become one of the country's most pressing health issues. The UK government responded with investigations such as the 1901 Royal Commission on human and animal TB, a clear sign of how serious the situation had become (UKRI, 2025). When TB became a notifiable disease in 1913, the numbers were staggering—over 117,000 new cases in England and Wales that year alone. Over time, that number began to fall, dropping to just over 5,000 by the late 1980s. However, things changed again: TB cases climbed by 65%, peaking in 2011 with 8,411 reported cases. This shift was partly due to changes in who TB was affecting—high-risk groups became more vulnerable than the general population (Department of Health, 2018).
Vaccination has played a big part in TB prevention. The BCG vaccine was introduced in 1953, first given to teenagers, then later focused on protecting infants at higher risk, especially children born into communities with higher TB rates or recent migrants from countries with more cases. Today, it is part of a risk-based immunisation strategy (Department of Health, 2018).
Efforts to detect TB have also evolved. The UK now uses screening programmes, community outreach, and tests for certain visa applicants from higher-risk countries (NICE, 2018; UK Health Security Agency, 2024). Still, in 2023, TB cases rose again, up 11% from the year before, to 4,855 diagnoses (UK Health Security Agency, 2024). In 2025, TB is still deeply linked to social inequality. People living in more deprived areas, including asylum seekers and those experiencing homelessness—especially adolescents—remain the most affected (UK Health Security Agency, 2024).
Key Concepts / Mechanisms – What It Is, How It Works
Tuberculosis is caused by the infectious agent Mycobacterium tuberculosis (M. tuberculosis). It enters the human body via the respiratory tract, and specialised immune cells in the lungs (macrophages and dendritic cells) engulf it. Then, TB reproduces as infected immune cells pass it to other cells, triggering a chronic inflammatory immune response (Granulomas). These granulomas can rupture, releasing TB bacteria into the airways, which spreads the TB to others (Yang et al., 2023).
Therefore, the primary mode of contracting TB is through droplets from an infected individual. However, an individual cannot contract TB as easily as with a common cold (Long, Divangahi, and Schwartzman, 2022). There are additional factors that increase the likelihood and are primarily associated with the symptoms and overall health of the TB spreader (the infected individual), as well as with characteristics of the environment where the TB spreader and an individual interact, as shown in the graphic below.
Graph 1. Additional factors that increase the likelihood of getting infected with TB

Another characteristic of TB that makes it challenging to identify and treat is its unusual bacterial behaviour, in which infection symptoms can pass unnoticed, delaying immediate treatment. Immediately after infection with TB, individuals can be active spreaders (active TB), with visible symptoms, or inactive/latent spreaders (latent TB), with no visible symptoms; therefore, infection is not spreadable (Price and Nguyen, 2024). The graphic below highlights the differences between active and latent TB.
Graph 2. Latent vs Active TB
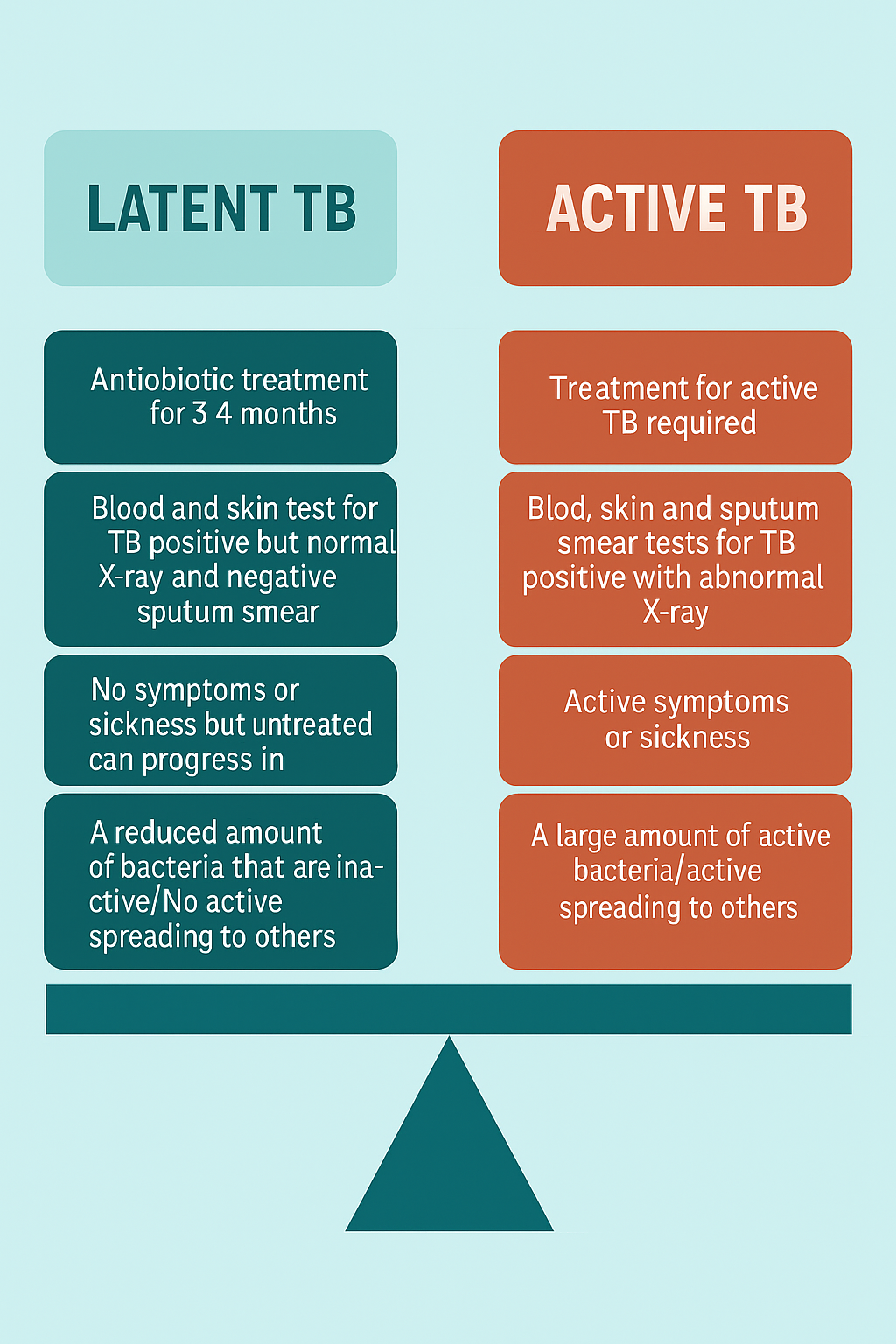
As shown in the graphic above, the diagnosis and treatment of TB vary depending on whether it is latent or active. Moreover, inactive TB present the most significant challenge as it cannot be diagnosed or treated as it cannot be easily observed. Currently, standard tests worldwide used to identify TB (but do not establish if it is active or latent) are the tuberculin skin test (TST) and interferon gamma release assays (IGRAs). The standard treatment involves antibiotics for several months; however, many patients find the side effects and the treatment's duration challenging. One of the main challenges for TB treatment is the continued increase of Multidrug-resistant TB (MDR-TB). Despite the slowdown and downsizing trend at the global level, MDR TB caused an estimated 150,000 deaths globally in 2023 (World Health Organisation, 2024). At the UK levels, for 2023, the UK Health Security Agency reported 34,0% of individuals with culture-positive disease (UKHSA, 2025).
Examples / Applications – Real-World Cases
In 2023, TB rates were more than four times higher in the most deprived areas of England compared to the least deprived (UK Health Security Agency, 2024). Although this so-called 'Victorian' illness seems more like a news item than an active threat to local communities, from 2024 to the current date of 2025, several local outbreaks have shown how quietly yet swiftly cases are reaching neighbourhoods. Here can be mentioned: Meridian Community Primary School in Peacehaven (Stock, 2025); University of Salford, Manchester (The University of Salford, 2023); Morgan Academy Dundee (Simpson, 2025). The UK approach toward TB is multilateral and multidimensional, involving multiple agencies and is guided by the WHO elimination target set for 2035 (UK Health Security Agency, 2023).
Figure 1. Proportion of culture confirmation among TB notifications in London by site of disease, over the 2 years (last 8 quarters) (Source: UK Health Security Agency, 2025a)
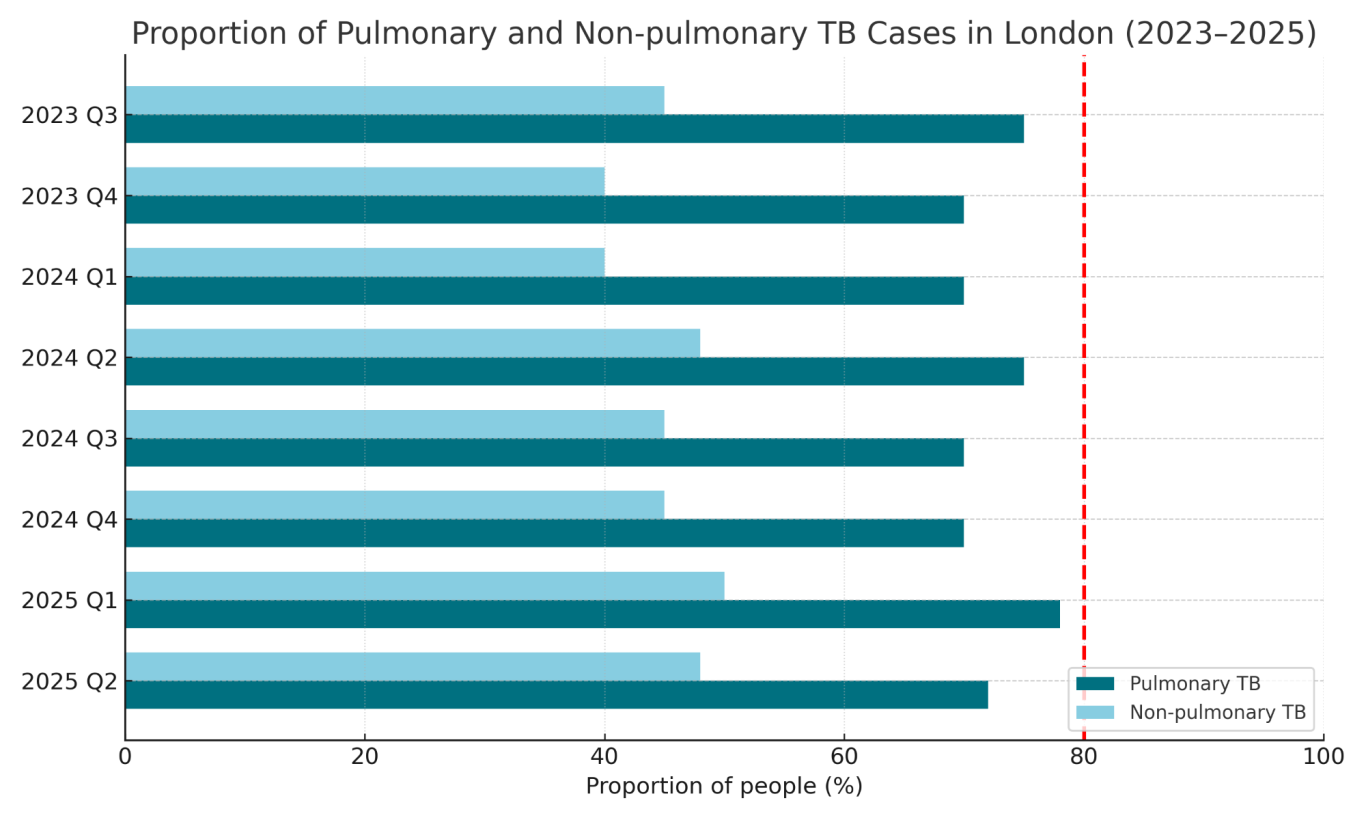
In 2023, TB rates were more than four times higher in the most deprived areas of England compared to the least deprived (UK Health Security Agency, 2024). Although this so-called 'Victorian' illness seems more like a news item than an active threat to local communities, from 2024 to the current date of 2025, several local outbreaks have shown how quietly yet swiftly cases are reaching neighbourhoods. Here can be mentioned: Meridian Community Primary School in Peacehaven (Stock, 2025); University of Salford, Manchester (The University of Salford, 2023); Morgan Academy Dundee (Simpson, 2025).
The UK approach toward TB is multilateral and multidimensional, involving multiple agencies and is guided by the WHO elimination target set for 2035 (UK Health Security Agency, 2023).
Graph 3. The UK approach to TB
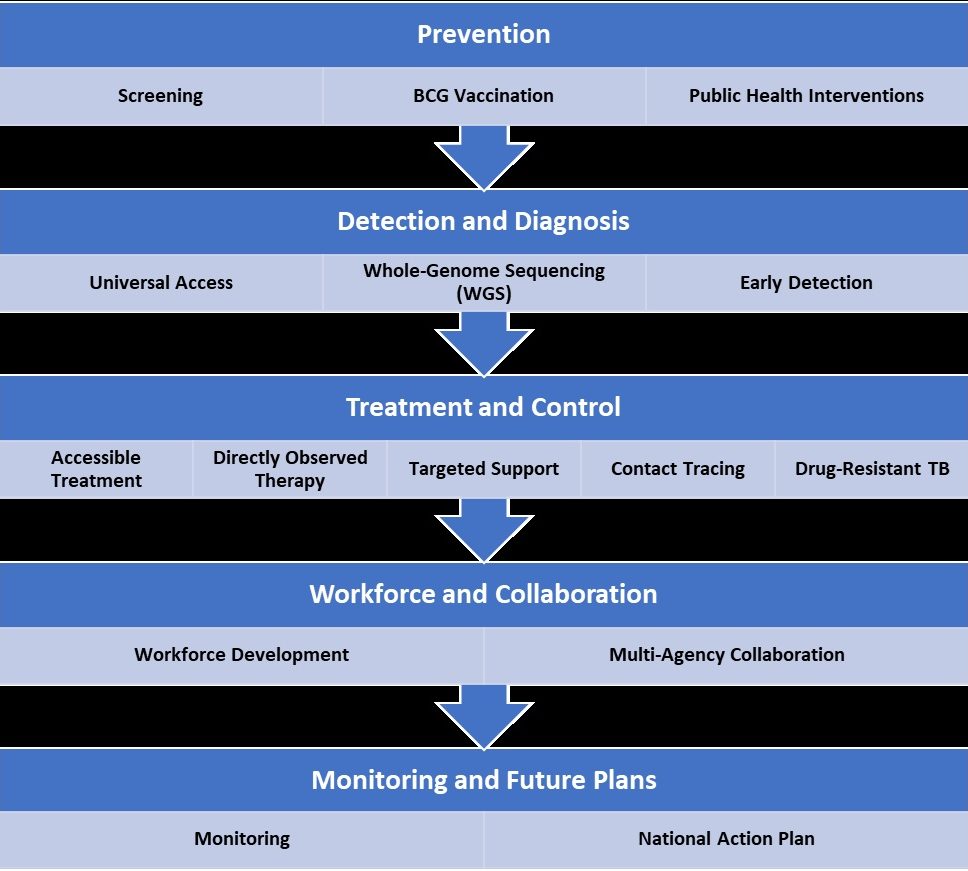
Implications / Takeaway
TB has a significant impact on NHS resources due to its long treatment duration and ongoing monitoring and tracing (Allen, 2025). TB remain a problem in the UK due to its linkage to poverty, where social risk factors make people vulnerable to illness and hinder the treatment continuity, as a third of people with TB in England start their treatment around 4 months later than recommended (Millington et al., 2025). Moreover, the stigma around TB is still an impediment in seeking treatment, plus underdiagnosis due to unclear symptoms and inconsistent diagnostic services around regions (Allen, 2025).
The UK Health Security Agency's current idealistic targets seem tailored to the healthcare sector rather than reaching people in the environments where people are born, grow, live, work, and age (Millington et al., 2025). Access to high-quality TB care, an enhanced screening approach, and a modern, accurate data system for TB are among the elements that need to be addressed immediately (Allen, 2025).
Improving the evidence base for TB prevention remains a priority for national research funding, as its prevention and treatment have been demonstrated to be worth the investment through social benefits achieved and long-term cost savings (Allen, 2025). Moreover, TB must remain on the Public Health Research and Policy Agenda as part of social justice for the UK's population, aiming to improve their health. Moreover, TB remains a public health priority requiring sustained academic and policy focus (Millington et al., 2025).
References
Allen, M. (2025) RNOH/GIRFT Review of Tuberculosis National Report. Available at: https://www.england.nhs.uk/wp-content/uploads/2025/03/girft-review-of-tuberculosis-national-report.pdf (Accessed: 10 November 2025).
Barberis, I., Bragazzi, N., Galluzzo, L. and Martini, M. (2017) ‘The history of tuberculosis: from the first historical records to the isolation of Koch’s bacillus’, Journal of Preventive Medicine and Hygiene, 58(1), pp. E9. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC5432783/ (Accessed: 9 July 2025).
Bournemouth University (2021) Earliest known case of TB in Britain on display in Wimborne. Available at: https://www.bournemouth.ac.uk/news/2021-01-13/earliest-known-case-tb-britain-display-wimborne (Accessed: 9 July 2025).
Cooper, R.G. (2008) ‘Human tuberculosis in colonial Victorian and present-day Britain’, Journal of Pre-Clinical and Clinical Research, 2. Available at: https://www.jpccr.eu/pdf-71289-8518 (Accessed: 17 July 2025).
Department of Health (2018) Chapter 32: Tuberculosis. In: Immunisation against infectious disease – ‘The Green Book’. Available at: https://assets.publishing.service.gov.uk/media/5b645a2140f0b66875559e93/_Greenbook_chapter_32_Tuberculosis_.pdf (Accessed: 22 July 2025).
GOV.UK (2018) Tuberculosis screening. Available at: https://www.gov.uk/guidance/tuberculosis-screening (Accessed: 22 July 2025).
Long, R., Divangahi, M. and Schwartzman, K. (2022) ‘Transmission and pathogenesis of tuberculosis’, Canadian Journal of Respiratory, Critical Care, and Sleep Medicine, 6(sup1), pp. 22–32. doi: https://doi.org/10.1080/24745332.2022.2035540.
Millington, K.A. et al. (2025) ‘Addressing the Growing TB Disease Burden in England’, The Lancet Respiratory Medicine, 13(5). doi: https://doi.org/10.1016/s2213-2600(25)00088-8.
NICE (2025) Tuberculosis. Available at: https://bnf.nice.org.uk/treatment-summaries/tuberculosis/ (Accessed: 9 July 2025).
Price, C. and Nguyen, A.D. (2024) Latent Tuberculosis. Available at: https://www.ncbi.nlm.nih.gov/books/NBK599527/ (Accessed: 15 September 2025).
Simpson, J. (2025) Tuberculosis case confirmed at Dundee Secondary School. Available at: https://www.thecourier.co.uk/fp/news/5229941/tuberculosis-morgan-academy-dundee/ (Accessed: 8 November 2025).
Stock, A. (2025) Sussex primary school staff member diagnosed with serious disease. Available at: https://www.theargus.co.uk/news/25052241.sussex-primary-school-pupil-diagnosed-historically-deadly-disease/ (Accessed: 8 November 2025).
The University of Salford (2023) Confirmed case of tuberculosis (TB) on campus. Available at: https://www.salford.ac.uk/news/confirmed-case-of-tuberculosis-tb-on-campus (Accessed: 8 November 2025).
Tobin, E.H. and Tristram, D. (2024) Tuberculosis. Available at: https://www.ncbi.nlm.nih.gov/books/NBK441916/ (Accessed: 9 July 2025).
UK Health Security Agency (2022) What is TB and what are we doing to combat it? Available at: https://ukhsa.blog.gov.uk/2022/03/23/what-is-tb-and-what-are-we-doing-to-combat-it/ (Accessed: 16 July 2025).
UK Health Security Agency (2023) Tuberculosis (TB): Action plan for England, 2021 to 2026. Available at: https://www.gov.uk/government/publications/tuberculosis-tb-action-plan-for-england (Accessed: 8 November 2025).
UK Health Security Agency (2024) Tuberculosis in England, 2024 report. Available at: https://www.gov.uk/government/publications/tuberculosis-in-england-2024-report/executive-summary (Accessed: 22 July 2025).
UK Health Security Agency (2024) Tuberculosis incidence and epidemiology, England, 2023. Available at: https://www.gov.uk/government/publications/tuberculosis-in-england-2024-report/tuberculosis-incidence-and-epidemiology-england-2023 (Accessed: 9 July 2025).
UK Health Security Agency (2025a) National quarterly report of tuberculosis in England: quarter 2, 2025, provisional data. Available at: https://www.gov.uk/government/statistics/tuberculosis-in-england-national-quarterly-reports/national-quarterly-report-of-tuberculosis-in-england-quarter-2-2025-provisional-data (Accessed: 26 September 2025).
UK Health Security Agency (2025b) UKHSA launches call for evidence to tackle rising TB. Available at: https://www.gov.uk/government/news/ukhsa-launches-call-for-evidence-to-tackle-rising-tb (Accessed: 9 July 2025).
UKHSA (2025) Tuberculosis diagnosis and microbiology, England, 2023. Available at: https://www.gov.uk/government/publications/tuberculosis-in-england-2024-report/tuberculosis-diagnosis-and-microbiology-england-2023 (Accessed: 23 September 2025).
UKRI (2025) History of MRC. Available at: https://www.ukri.org/who-we-are/mrc/who-we-are/our-history/ (Accessed: 16 July 2025).
World Health Organization (2024) 1.3 Drug-resistant TB. Available at: https://www.who.int/teams/global-programme-on-tuberculosis-and-lung-health/tb-reports/global-tuberculosis-report-2024/tb-disease-burden/1-3-drug-resistant-tb (Accessed: 23 September 2025).
Yang, J., Zhang, L., Qiao, W. and Luo, Y. (2023) ‘Mycobacterium tuberculosis: Pathogenesis and therapeutic targets’, MedComm, 4(5). doi: https://doi.org/10.1002/mco2.353.
